Mohamad-Ali Salloum is a Pharmacist and science writer. He loves simplifying science to the general public and healthcare students through words and illustrations. When he's not working, you can usually find him in the gym, reading a book, or learning a new skill.
Efficacy Vs Potency
Share
What are they and what do we need to know about these two concepts?
First let’s define them.
Efficacy is the ability of a drug to elicit a physiologic response when it interacts with a receptor.
Potency is the amount of drug needed to produce a certain response.
Two drugs can have the same effectiveness but different potencies.
Let’s suppose we have 2 dugs, Drug A and Drug B.
Drug A induces a 70% effect with only 3 molecules.
Drug B induces the same 70% effect with 6 molecules.
This means that both has the same efficacy, but Drug A is more potent than Drug B.
Knowing the difference in potency between drugs allows us to have several options for treating a patient and achieving the same clinical results.
Note that some drugs (let’s say Drug C) can’t reach the 70%, and when used in their maximal concentration they may reach 50% effect. In comparison with both Drugs A and B, Drug C is considered less effective.
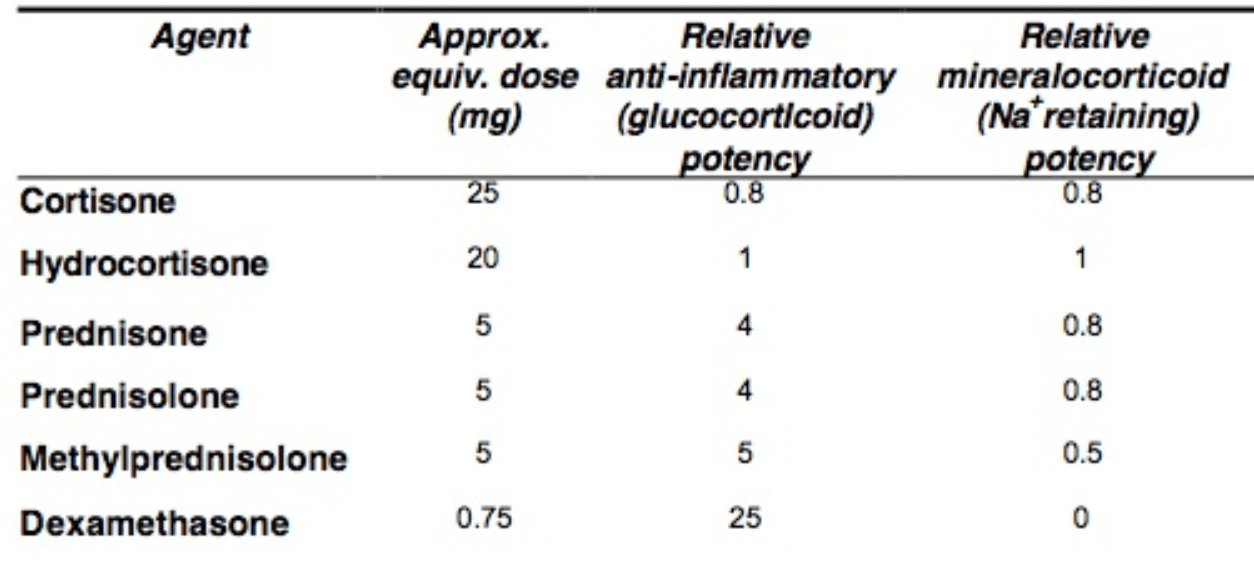
For example, when comparing the corticosteroids (as shown in the table below), we find that dexamethasone is the most potent in terms of anti-inflammatory effect. However, all of the below corticosteroids can achieve the same efficacy when used at the appropriate calculated doses.
You can also watch the illustrative video below for more understanding of the topic.
List of Services
ABOUT THE AUTHOR
Mohamad-Ali Salloum, PharmD
Share
Recent articles:





















